What is diabetes mellitus (DM)?
Diabetes mellitus, or simply diabetes, is a group of metabolic diseases in which a person has high blood sugar, either because the pancreas does not produce enough insulin, or because cells do not respond to the insulin that is produced. Insulin controls the amount of glucose (sugar) in the blood.
Diabetes is a serious condition that affects all ages and both males and females.
Both Type 1 DM and Type 2 DM, once developed, are life-long conditions. There is no known cure but all types of diabetes can be treated effectively.
Main types of diabetes mellitus (DM)
Type 1 DM is an autoimmune disease in which the body attacks and destroys the beta cells that produce insulin inside the pancreas. The body then fails to produce insulin. This form of DM usually occurs in young children or adolescents but can occur at any age.
Type 2 DM results from insulin resistance, a condition in which cells fail to use insulin properly, sometimes combined with an absolute insulin deficiency. This form has been referred to historically as “adult-onset diabetes” but now is appearing in children as young as eight or even younger.
Gestational diabetes occurs when pregnant women without a previous diagnosis of diabetes develop a high blood glucose level. Gestational diabetes increases the risk of type 2 onset later in life for both mother and child.
There are other rare forms of DM including congenital diabetes, due to genetic defects of insulin secretion, monogenic diabetes caused by an abnormality in one of several genes, and other forms of DM related to cystic fibrosis and high doses of steroids.
“Pre-Diabetes” refers to the condition in which blood glucose levels are higher than normal but not high enough to be diagnosed as T2DM. Not everyone with pre-diabetes will develop T2DM but many with pre-diabetes are at much higher risk of developing T2DM.
Symptoms of T1 DM |
Symptoms of T2 DM |
| * Unusual thirst
* Frequent urination * Extreme fatigue or lack of energy * Blurred vision * Constant hunger * Sudden weight loss * Bedwetting |
* Unusual thirst
* Frequent urination * Extreme fatigue or lack of energy * Blurred vision * Tingling or numbness in hands and feet * Frequent or recurring fungal infections * Cuts and bruises that are slow to heal |
If you show these signs, you should seek medical attention. These signs can be mild or absent in people with ‘early stage’ T2 DM. T2 DM can go unnoticed and undiagnosed for years. Thus, at time of diagnosis, cell damage can be in progress. T2 DM is also ‘progressive’. It is estimated that 40% of those living with T2 DM do not know they have it.
Early identification and timely treatment of diabetes are essential, as well as blood pressure control and lifestyle factors such as smoking cessation, maintaining a healthy body weight, healthy eating and regular exercise.
T1 DM requires multiple daily injections of insulin in combination with attention to proper diet, regular exercise, and regular blood sugar monitoring
T2 DM may be controlled with diet and exercise but oral medication may also be required. In some cases, insulin may become necessary eventually. Recent experience indicates that some youth with T2 DM are not responsive to oral medication alone and also require insulin at the outset. Effective management of T2 DM also requires regular blood sugar monitoring.
Gestational diabetes usually resolves after delivery but mothers remain at increased risk of developing T2 DM later in life as does their baby.
It is important to ask your healthcare provider to test you for diabetes. That normally starts with a simple ‘blood glucose level’ test which is immediate and involves only a small pin prick. If the results indicate a potential problem, further testing will be required.
Why do you need insulin?
Every living cell in your body requires energy so you can think, work and play. The starting source for that energy is the food you eat and food needs to be ‘broken down’ or digested into basic parts in order to be absorbed and used in the body.
Carbohydrates (carbs) are of special interest because they are ‘broken down’ into simple sugars of which ‘glucose’ is critical as a source of energy. The amount or ‘level’ of glucose in your blood is very important for good health. Your ‘blood glucose’ level depends on a delicate balance that is maintained by several organs working together in harmony.
Control of the amount of glucose in the blood depends on two hormones, insulin and glucagon, that are produced and secreted by the pancreas.
Insulin is produced by the beta cells in the pancreas. The alpha cells of the pancreas produce glucagon.
Insulin controls the amount of glucose (sugar) in the blood.
Glucose is absorbed into your blood and carried around your body for distribution to the cells that need it. But, for those cells to take in glucose, they must first be ‘unlocked’ and the key required for that is called ‘insulin’.
If you have diabetes, your pancreas does not produce insulin, or enough insulin, or your cells can be ‘resistant’ to insulin.
When those circumstances happen, glucose builds up in your bloodstream and your cells face a shortage of energy. Different cells react in different ways and that is why there is a rather long list of ‘symptoms’ that can arise with diabetes. For example, the need for frequent urination is a result of your body trying to flush the excess glucose.
Glucose imbalance
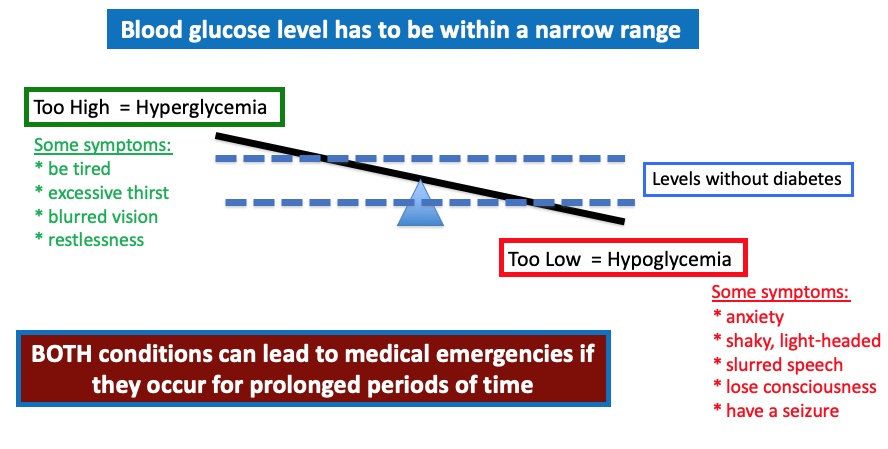
Your blood glucose level has to be within a narrow range and the level depends on a delicate balance that is maintained by organs working together in harmony; in particular the pancreas and the liver.
When blood glucose levels increase, after eating for example, insulin is secreted from the pancreas and triggers cells to take glucose from the blood stream and convert it to energy. At the same time, insulin triggers the liver to convert and store glucose as glycogen for future use when blood glucose levels decrease.
When blood glucose levels decrease, between meals for example, glucagon is secreted and triggers the body to convert glycogen, which is stored in fat, liver and muscles, to glucose and release it into the blood stream.
If the amount of glucose in the blood is too high, the result is a condition called hyperglycemia. The opposite situation, where glucose is too low, is known as hypoglycemia.
Repeated or persistent glucose imbalance, hypo- or hyperglycemia, sets the stage for permanent cell damage and the onset of diabetes complications. In extreme cases, both can lead to medical emergencies.
This combination of glucose, hormones and organs represents a very elegant system but one that needs to stay in a proper range of balance.
Serious complications can arise if diabetes of any type is left untreated
Diabetes can increase your risk of:
- Heart disease and stroke
- Kidney disease
- Eye disease and blindness
- Neuropathy (nerve damage)
- Vascular disease leading to risk of lower limb amputation
- Dental disease
- Anxiety, depression, eating disorders and Diabetes Stress
- Erectile dysfunction (impotence)
Diabetes, Obesity and Mental Illness in Youth
Diabetes is a worldwide pandemic affecting all countries and all ages and the numbers are growing annually. Included in that is an increasing number of youth living with diabetes. There is a strong correlation between obesity and the rise of Type 2 diabetes in youth. Similarly, there are interactions between mental disorders in youth and diabetes. These conditions also are appearing increasingly in various combinations in youth.
Diabetes, mental disorders and obesity in youth each have significant common characteristics:
- increasing prevalence and earlier onset
- systemic barriers to access for health card
- highly variable capacity for, and quality of, support for transition from pediatric to adult healthcare
All three conditions require broader awareness of the risks and early intervention. Together, they represent a ‘perfect storm’ for our youth.
